In Sub-Saharan Africa, 93% of people lack access to safe surgical care when needed. A significant contributing factor in this is the acute lack of surgical care providers.
The RCSI Institute of Global Surgery works to improve access to high-quality, essential surgical care for underserved populations. Since 2007, RCSI has supported the College of Surgeons of East, Central and Southern Africa (COSECSA) to advance surgical training in the region, with the support of Irish Aid.
Supported by the collaboration programme, COSECSA has grown to be the largest single contributor to the surgical workforce in the East, Central and Southern Africa region.
Given the vast size of the region, technology plays a highly important role in enabling COSECSA to deliver a common training programme across 20 countries. RCSI and COSECSA have partnered to develop a number of tools for e-learning, training programme management and much more.
The COSECSA electronic surgical training logbook is a great example of how technology is used to support surgical training in the region.
The e-logbook is a bespoke piece of software developed by RCSI colleagues in Surgical Affairs in collaboration with the Irish software company Tekenable. It allows surgical trainees to record all of the procedures that they perform, or with which they assist, and has recently recorded its 500,000th operation.
The e-logbook was developed specifically for low-resource environments. It is an important tool for trainees themselves, but also vital for the evaluation and quality assurance of over 1,000 trainees, who are training in 135 accredited hospitals across 20 countries. It is understood to be the largest dataset of African surgical data ever assembled.
Prompt intervention
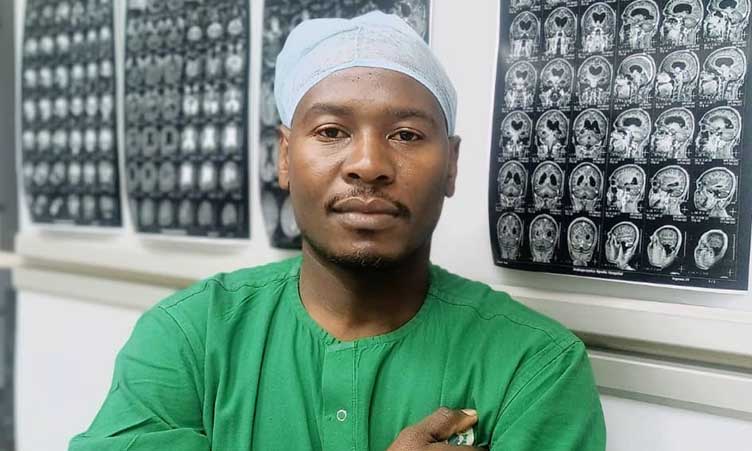
Dr Aaron Munkondya, a neurosurgeon from Zambia, performed the 500,000th procedure, which was the emergency insertion of a ventriculo-peritoneal shunt (VPS) for a five-year-old male. At the time of the procedure Dr Munkondya was a trainee neurosurgeon. He graduated as a neurosurgeon from COSECSA in December 2023.
The procedure was carried out in the University Teaching Hospital in Lusaka, the capital of Zambia. Dr Munkondya explained: “This is a cerebrospinal fluid (CSF) diversion procedure, which we do in patients with hydrocephalus. It can come about due to a problem with CSF absorption, blockage along its pathway or over-production. This leads to enlargement of the ventricles and pressure buildup in the head, which we overtly see as a big head in children especially those less than two years.
“It causes severe headaches, vomiting, seizures, reduced levels of consciousness as well as regression of milestones among other clinical features, especially those children whose fontanelles are closed, and this is what this child came with. The clinical picture and image findings called for prompt intervention.
“Surgery was very important to stop further deterioration in this child and to halt the progression of the disease, because eventually it will lead to death if it's not done… if it is done too late, permanent neurological damage in the child could have occurred, and the child may never sit, walk or see again. So we try to intervene as soon as we can to prevent further loss of function and improve the overall clinical outcome in the patient.”
This procedure is common in Zambia, just like any other resource-limited country. Dr Munkondya explained that partially treated meningitis can lead to post-infectious hydrocephalus, and that babies with congenital infections (toxoplasmosis, rubella, cytomegalovirus (CMV) and herpes simplex virus (HSV), and those born prematurely can have this type of condition.
There are also many challenges such as patients presenting late to hospital and arriving from far-flung regions, with no proper transport to the hospital. This means that the condition is often treated late.
Timely, accessible and affordable surgical care
Patients in low-resource countries, like Zambia, have less timely access to surgical care than people in better-resourced countries. By increasing access to surgery in the local community, and providing home-grown solutions rather than venturing outside the region, patients benefit from quicker and more affordable care. Local care is also better value for government, allowing for funds to be used more efficiently.
Growing up in Zambia, Dr Munkondya looked to engineering firstly, but became passionate about biology in secondary school. The desire to alleviate suffering, including that of his sister, who has asthma, led him to pursue medicine. He hopes to specialise in a spine or paediatric subspecialty.
Locally the team is growing with more than ten practising neurosurgeons who are building more subspecialties. He envisions pushing for a paediatric hospital where patients can be served better, with more equipment making hospitals more efficient and effective.
Dr Munkondya is one of 64 Zambian surgeons to have graduated from COSECSA. Research shows that 93% of surgeons trained in region remain in the region. They perform on average 300-400 major surgeries a year and become trainers for the newer generation of surgeons.
They provide timely, accessible and affordable surgical care in communities that would have previously had great difficulty accessing the care they needed. This care is not just improving the health of people in the community, but is also contributing to the local economy by allowing patients to return to work. This, in turn, improves health outcomes.
Find out more about the work of the RCSI Institute of Global Surgery here.
RCSI is committed to achieving a better and more sustainable future through the UN Sustainable Development Goals.
![]()
![]()